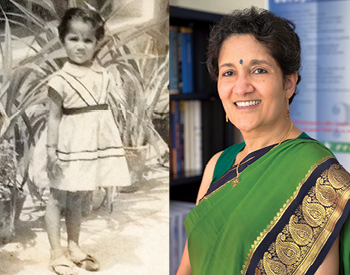Balancing Acts
By Dana Goldman

Steven Mets was born with a rare congenital heart defect called Shone’s complex and has a pacemaker, a bovine valve, and a mechanical valve.
Steven Mets is used to blending in—and being misunderstood.
After all, he seems like a typical 21-year-old college student, into gaming and the outdoors. "I've had doctors look at me like, 'Why are you here? You're fine,' " says Mets, a student at Clemson University.
But in his case, appearances are deceiving.
Look more closely and there are clues that Mets is, in many ways, exceptional. Take the scars on his body, remnants of a series of heart surgeries that started when he was just four days old (and that he expects will someday include a heart transplant.) Or his panoply of pills, the type of medications usually prescribed to much older adults. You might see his roommates lifting heavy objects for him, or, until recently, slowing down when walking up hills to make sure he could keep up.
Mets was born with a rare congenital heart disease called Shone's complex, involving multiple cardiac defects. He has a pacemaker, a bovine valve, and a mechanical valve that all help keep his heart going.
|
|
He is one of a growing number of adults now living with congenital heart defects (CHDs) that, a few decades ago, would have been a sure death sentence. "Someone who was born in the 1950s with a heart defect—just about any heart defect that wouldn't spontaneously resolve—their chances to survive to adulthood were poor," says Wendy Book, Mets's cardiologist and director of Emory's Adult Congenital Heart Center.
Patients with a hole in their heart or a missing chamber would rarely age out of a pediatric practice and grow up to need adult health services. But in the past few decades, a series of medical advances began extending these children's lives, sometimes just for a few years—and then a few more.
Treatment is advancing so rapidly that even a five-year fix will often buy the patient enough time that a new treatment is available when the last one stops working. "That can make a huge difference in giving them a chance at the life they want so badly," Book says.
When the first wave of children with CHD grew too old for pediatric cardiology services, they sometimes found themselves out of competent medical hands. "Nobody was prepared to take care of them when they grew up," says Book, a professor of medicine at Emory.
Cardiologists specializing in adults are trained to help patients with blocked arteries and cardiovascular disease. As Mets discovered, most had rarely if ever seen a patient with unusual circulation, valve problems, or only one pumping chamber of the heart, and the complications caused by these structural issues. If adult patients with heart defects required surgery, they often ended up back at a pediatric hospital with a pediatric cardiac surgeon.
The amount of care these patients require is both time-consuming and expensive. "But when you're talking about people with 50 years ahead of them, how can you not put forward the resources to help?" asks Book.
Attention is being paid: Congress passed the Congenital Heart Futures Act in 2010, a law that provides funding for Centers for Disease Control and Prevention (CDC) tracking across a patient's lifespan. And adult congenital heart disease has become a new subspecialty in internal medicine, with the first board exams scheduled for 2015 by the American Board of Internal Medicine.
|
|
Emory's Adult Congenital Heart Center, designed at the turn of the millennium to serve the growing number of patients older than 18, is one of a handful of such emerging centers around the country and the only one in Georgia.
"The challenges are infinite," says Book. "These patients are often in the first wave for surgical procedures. We work without knowledge of long-term outcomes. The defects are all very rare and very different. Everything about them is unique and we are often faced with doing procedures that have never been done before because a patient's situation calls for it."
Mets knows how tough it can be. He prioritizes his medical care even when it means driving the 120 miles to Emory during a busy week at college. Even so, there are continual dangers. Two years ago, he came down with pneumonia. "My heart wasn't strong enough to handle it," he says. "My condition kept getting worse." His liver and kidneys began to fail. Book had planned to replace his failing aortic valve with a bovine valve after his recovery, but decided Mets's only chance was to go ahead and replace the valve immediately.
Conducting open heart surgery on a patient with cardiac defects and pneumonia is anything but easy. It took three attempts to replace Mets's aortic valve. During the last attempt, he went into cardiac arrest twice. At one point, his heart stopped pumping enough blood to keep his organs going. The surgery was so fraught that doctors decided to keep him unconscious and on life support for a few weeks after the procedure in hopes that this would take pressure off his heart and allow it to heal. "Against all odds, I eventually woke up," Mets says.
Months of physical rehabilitation followed before he was strong enough to return to college. "I've had more close calls than I would like," he says.
Since recovering from his last aortic valve replacement, he can walk up hills without stopping for the first time in many years. "I now have better heart function than I've ever had," says Mets, who is majoring in computer science and conducting research on virtual reality. "I have a lot of hope that I'll wind up with a long and full life."
Which is exactly what Asha Krishnaswamy, an IT specialist at the Centers for Disease Control and Prevention (CDC), is doing—flourishing as a wife, mother, and professional, against all odds.
She was born with the congenital heart defects collectively called tetralogy of Fallot and wasn't expected to live past her teens. "Most kids today have correction surgery within the first six months of life," she says. "But nearly 40 years ago, they didn't have that surgery."
Instead, Krishnaswamy's early life in India was confined by clear warnings from her parents and doctors about what was and was not safe for her to do. "I had a lot of dos and don'ts," she remembers. "One of them was not to ride a bike. I've never been on a bike." Embarrassed by her scars, she avoided swimming into her late 20s.
Now at 55, she has received care for her condition across three continents (India, England, and the U.S.) and is a survivor of four heart surgeries. Krishnaswamy has been coming to Emory for treatment since 2005 and no longer worries about what others might think when they see her scars. "I show them as a badge or an emblem," she says, laughing. "It's like beating nature."
|
|
She is paying her good fortune forward, working at the CDC's Center for Birth Defects and partnering with Book on a longitudinal study of patients with cardiac defects. "We're looking at the population from a public health perspective," says Book.
Adds Krishnaswamy, "We don't know how many such individuals there are—the prevalence, the incidence, the racial profile. I'm trying to develop an algorithm to identify congenital heart disease."
After identifying patients, the next step is to follow them to see how different procedures impact their lifespan and quality of life.
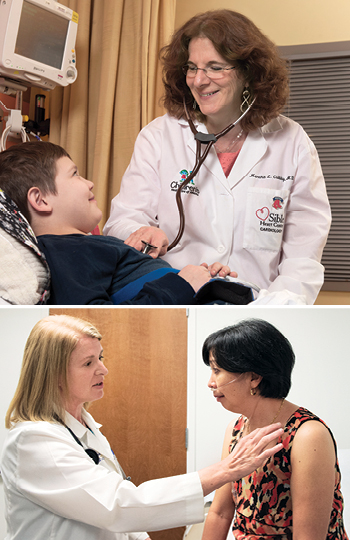
Proactive, consistent care from the very beginning is critical for children with CHD, says Martha Clabby, pediatric cardiologist and director of the Sibley Complex Congenital Heart Disease program, a decade-long collaboration between Emory and Children's Healthcare of Atlanta.
Clabby and her team care for infants who often require surgery immediately after birth. "Some of these babies are diagnosed prenatally," she says. "Parents might not even be able to hold the baby before they get airlifted here to start treatment."
The program began after Clabby's team noticed that despite good surgical outcomes, babies born with CHD still experienced a higher than normal incidence of sudden death once they left the hospital.
"One of the really important things when you have an at-risk patient population is for them to know they're at risk," says Clabby, an assistant professor of pediatrics who also directs the cardiac step-down unit at Children's Healthcare. "So our program involves an intensive parent education process that takes a multidisciplinary approach."
Teams include physicians, nurses, social workers, physical therapists, outpatient nurses, and special nurse educators who provide extensive one-on-one teaching about what is wrong with the babies and what parents need to do if they see something amiss.
Part of this instruction is emphasizing to parents, and later, the patients themselves, a difficult fact about CHDs: there is no perfect fix.
Doctors can work around defects, but rarely can the complications be fully mitigated, says Clabby. "If someone is born with half a heart, we can crudely mimic what the normal blood flow is, but not restore normal physiology," she says. "You can't create chambers of the heart that aren't there—at least not yet. But we use what we can to make things as normal as possible."
Clabby and her team have established procedures that are being picked up by other specialty centers around the country through their participation in the Joint Council of Congenital Heart Disease. Since 2004, these steps have dramatically decreased the rate of sudden deaths among young patients at Sibley. They include placing alerts on the patients' electronic healthcare records, making sure CHD patients are seen immediately if their families call, and educating families about the need for proactive care and vigilance.
Simple tactics are often the most effective. "Congenital heart disease patients literally have a blue sticker on their hospital room door that says they're high risk so that anyone walking by, whether it be a cardiologist or a social worker, should respond in even more of an acute way than we already do with our other patients," says Clabby.
And while she is realistic about the challenges her patients face—many will need three open heart surgeries before the age of four—Clabby says the work offers long-term rewards. "It's not enough to get a child to survive, right?" she asks. "That's great as a first step, but really what we want is to provide functional and happy lives for these kids. Getting them through the first years is just the beginning. To see them outside the hospital doing well—playing soccer or taking prom pictures—that's extremely gratifying."
Such success brings its own problems, however. "Many of our young adult patients have the perception that if they feel fine they don't need care," says Book. "They're busy—going to college, getting married, starting a career. Then, later, they come in during a crisis with an acute problem or when they're pregnant."
Up to 40 percent of patients with cardiac defects nationally fail to make the transition from pediatric to adult care.
That's where Fred "Rusty" Rodriguez III comes in, the rare cardiologist trained to work with both children and adults. His rounds regularly take him to hospitals including Egleston, Scottish Rite, Northside, and Emory.
On a recent Saturday morning, the Emory professor of pediatrics and internal medicine found himself in a back room at the arcade game center Dave & Buster's, talking about everything from sex to alcohol to life expectancy with a group of teens with congenital heart defects and their parents.
"How important is it to take my medications?" asks one.
"Can I get pregnant?" asks another.
All are curious to hear Rodriguez's answers about their own concerns.
These young adults might not stand out in a crowd. But all of them have a heart defect that requires regular monitoring and care.
"Some were born with holes in their heart," says Rodriguez. "Some with one functional pumping chamber rather than two. Some have problems with valves in their heart—either they're too narrow or too leaky. Some have large blood vessels coming off their heart in the wrong orientation."
Rodriguez and his team know that the more teens grasp about the seriousness of their condition, the greater responsibility they will take for their health, no matter how good they're feeling. "We want to encourage our teenagers to follow up with us their entire lives," he says.
Knowing what's wrong, what to do, what to look for, and what to anticipate is critical, says Clabby. "We have to balance giving families hope with being realistic about the dangers and need for chronicity of care."
An eventuality for some patients with congenital heart defects is a heart transplant. In a recent paper in the April 25 issue of Annals of Thoracic Surgery, Emory doctors David Vega, Wendy Book, and Brian Kogon, reported that of 12 adult patients who had a heart transplant because of a CHD at Emory Hospital between 2005 and 2013, all survived.
Such transplants are "challenging, fraught with adverse events, and require meticulous care and teamwork for success," the authors wrote. They attributed the high success rate to the transplants being performed by a surgeon specializing in congenital heart disease at an adult hospital, and to the post-operative care provided by both the congenital and the adult transplant teams.
"The strong relationship between Emory and Children's Healthcare enables us to collaborate and achieve outstanding results for our patients," says Kogon, chief of cardiothoracic surgery at Children's and associate professor of surgery at Emory's School of Medicine.
Teresa Harper, 62, may be one of the oldest women alive with her condition. At age 3, she was diagnosed with the rare congenital defect known as truncus arteriosus. The main blood vessel leaving her heart, the "truncus," failed to divide into the aorta and the pulmonary artery. She wasn't supposed to live past her teens but made it to her 40s before her heart and lungs began to fail. Doctors put her on the transplant list, and she resigned herself to life in a wheelchair. "I was in pretty bad shape," she says. "I couldn't even walk across a room without sitting down to rest."
She ended up at Emory's Adult Congenital Heart Center, and Book and her team saw something other doctors hadn't. "We noticed she had a loud continuous murmur, the type that suggested a 'kink' in one of the arteries to her lungs," says Book.
They decided to try an angioplasty to improve blood flow—something not done for patients like Harper even a decade ago. It increased her oxygen levels, improved her symptoms, and allowed her to be removed from the transplant list. A second angioplasty was also successful.
"Working with patients like Teresa is an honor and privilege," says Book. "From a medical perspective, they challenge us to come up with novel ways to improve a malfunctioning circulatory system and make it work better. From a personal perspective, these patients inspire us and teach us how to live fully."
Harper is now well enough to feed her chickens, teach piano, and work at her church.
And while she still can't walk long distances, she is able to indulge one of her biggest thrills. "I love to go to Six Flags, because I can ride those rides," she says. "I'll ride anything—the higher the better."
Down Syndrome and Congenital Heart Defects
|
|
The risk of congenital heart defects is greatly increased in babies with Down syndrome. About half of children with the genetic disorder have a heart defect, with atrioventricular septal defect (AVSD) being the most common.
Although sometimes it is possible to detect heart defects before birth through fetal ultrasound, the effects of an AVSD usually become apparent in the first few weeks of life. Often the clearest sign is difficulty feeding, says pediatric cardiologist Ken Dooley, associate professor of pediatrics: "The baby will feed one ounce and then go to sleep exhausted."
With AVSD, the central region of the heart separating the atria from the ventricles fails to form properly. Such defects can increase the workload on the heart, and a "complete" defect leads to heart failure: fluid buildup in the lungs and difficulty breathing, requiring surgery in the first year of life.
Before surgery, the goal is usually to have the child reach a weight of 11 pounds, Dooley says, at which point the risk of complications and poor outcomes are reduced. In the meantime, medications similar to those taken by adults with heart failure can help. Not all AVSDs are complete; some are milder and become apparent in the teenage years.
Emory researchers are taking part in a national study investigating the genetics of heart defects in the context of Down syndrome. Geneticists Stephanie Sherman, Michael Zwick, Lora Bean, and Tracie Rosser have been working with Dooley and colleagues across the country. "Studying congenital heart defects in the at-risk Down syndrome population can make it possible to reveal genes that impact the risk of heart defects in all children, including those with a typical number of chromosomes," Zwick says.
Folic acid taken during pregnancy can reduce the risk of some types of heart defects with Down syndrome, the researchers have found. Variations in genes connected with folic acid biology appear to play a role.
More recently, the team has found that infants with heart defects and Down syndrome are more likely to have rare, large genetic deletions. Those deletions tend to involve genes that affect cilia, cellular structures that are important for signaling and patterning in embryonic development. These findings, along with other recent studies, suggest that congenital heart defects can come from several genes and environmental factors, in addition to the substantial risk from extra chromosome 21."Our partnership with families who have a child with Down syndrome and our investment in a comprehensive clinical database and biorepository will continue to provide resources to study Down-syndrome associated conditions," Sherman says.